BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
URL: http://journal.zums.ac.ir/article-1-6809-en.html


 , Sevil Nasirmohtaram1
, Sevil Nasirmohtaram1 

 , Shadman Nemati *2
, Shadman Nemati *2 

 , Ehsan Kazemnezhad Leyli3
, Ehsan Kazemnezhad Leyli3 

 , Maliheh Akbarpour1
, Maliheh Akbarpour1 

 , Hedieh Ramezani1
, Hedieh Ramezani1 

 , Rastin Hosseinzadeh Asli4
, Rastin Hosseinzadeh Asli4 


2- Dept. of Otolaryngology, Head and Neck Surgery, Amiralmomenin Hospital, School of Medicine, Guilan University of Medical Sciences, Rasht, Iran ,
3- Dept. of Biostatistics, School of Nursing and Midwifery, Guilan University of Medical Sciences, Rasht, Iran
4- School of Medicine, Guilan University of Medical Sciences, Rasht, Iran
✅ Given the broad range and high incidence of disorders in the septum and lateral nasal wall, it is reasonable to routinely incorporate radiological investigations into the preoperative assessment of surgical candidates. This approach can potentially identify pathological findings, minimize postoperative complications, and optimize the surgical outcomes.
The nasal septum carries out several functions, such as splitting the nasal passage into two distinct compartments, maintaining the shape of the nasal dorsum, columella, and nasal tip. Disruptions, be it from injury or innate malformations, in the septum can result in substantial nasal obstruction and visible nasal deformities. The architecture of the nasal septum is composed of distinct osseous and cartilaginous elements, which encompass the perpendicular plate of the ethmoid bone (PPE), the vomer bone (VB), and the septal cartilage (SC). (1, 2). A flawless, undeviated septum ensures that incoming air is humidified, warmed, cleansed, and made appropriate for gas exchanges in the lung alveoli. However, a deviated septum can create various degrees of nasal blockage and modifications in nasal respiration (3). Disruptions in the airflow can result in olfactory impairment, impairment in the purification and humidification of respiratory air, and diminished oxygen intake. Additionally, anatomical aberrations in the septum can cause epistaxis (nosebleeds), chronic sinusitis, and commonly manifest as visible alterations in the nose's exterior appearance. Septum deviation indicates a departure from the midline, whether of the bone or cartilage, or both (4). This deviation may involve the cartilage, bone, or a combination of the two (5).
Common deformities associated with the septum include the subluxation of the rectangular cartilage from the maxillary ridge, or its deviations, which block the nasal floor and distort laminar airflow. This distortion can be traced back to early nasal trauma related to ridge fractures during childhood or simply due to cartilage growth and simultaneous narrowing of the maxillary ridge groove (6).
Septorhinoplasty is among the most frequently performed plastic surgeries and a common surgical procedure in the field of head and neck. Patients experiencing nasal blockages, where their grievances align with physical examination results, typically undergo septoplasty and turbinate surgery (7). Modern septoplasty techniques have evolved from simple septal cartilage manipulations and are usually combined with turbinate surgery. These procedures correct septal deformities to lessen nasal obstruction. Cosmetic and reconstructive rhinoplasty are recognized as being exceptionally delicate and simultaneously the most challenging plastic surgeries worldwide (8, 9). Combined septoplasty and rhinoplasty are instrumental in correcting nasal deviation and supplying cartilage grafts. Septoplasty is also performed in patients with severe epistaxis resulting from septal varices or severe deviation. The cause is typically a deviation of the anterior cartilage, which leads to turbulent airflow that causes the nose to collapse, resulting in nasal mucosa dryness and irritation (10).
Advancements in understanding the anatomy and physiological characteristics of the nose have paralleled the evolution of surgical remedies for obstructive nasal issues. The septum is recognized for its role in determining the shape and aesthetic of the nose, as well as its function in respiration (11).
Assessment of the septum's position should be carried out following all septum reconstruction surgeries and osteotomies. This is particularly crucial at the junction where the bone and cartilage of the nose converge. Here, surgeons can establish if there is sufficient dorsal support (12).
Typically, a single procedure of either septoplasty or rhinoplasty may not suffice for total nasal reconstruction. Thus, a combined approach is often adopted (13). Rhinoplasty stands as one of the most intricate procedures within the realm of plastic surgery (14). A minor modification of 1 mm can significantly affect the surgical result, necessitating an in-depth understanding of nasal anatomy and adjacent structures on the part of the surgeon (15). The surgical goal for these patients is to address both aesthetic and functional issues, ultimately enhancing their quality of life (16).
On each lateral wall of the nasal cavity, there are three bony projections known as nasal turbinates. In a condition known as concha bullosa, the turbinate has a double layer of bone instead of a single layer (17).
The anatomical configuration of the nasal cavity exhibits significant diversity among the general population, with some variations contributing to pathological conditions. Each variation or pathological condition demands a distinct therapeutic approach. This study investigates the prevalence of disorders of the septum and lateral nasal wall among patients undergoing septorhinoplasty at Amir-almomenin Hospital, a university-affiliated referral center located in Rasht, in northern Iran.
This observational study involved all prospective septorhinoplasty patients aged between 18-60 years, who presented to the Amir-Almomenin Hospital, an academic medical center located in Rasht, northern Iran, during the years 2011-2012. The participants were apprised of the study and provided informed consent, with an assurance of complete confidentiality of personal information. The recruitment strategy employed was convenience sampling.
We excluded participants who had a history of major craniofacial trauma or surgeries, conditions such as acromegaly or gigantism, fungal infections in the paranasal sinuses, craniofacial malignancies, chronic rhinosinusitis, saddle nose or crooked nose deformities, and congenital anomalies like cleft lip or cleft palate. Preoperative demographic and essential data were documented using a questionnaire. Intraoperative observations, including the location and nature of septal abnormalities (such as nasal ridge perforation, columellar dislocation, caudal septum deviation, septal cartilage fractures, deviations of the maxillary crest, high septal deviation, and spurred vomer), and characteristics of the lateral nasal wall (including lower turbinate hypertrophy, middle turbinate hypertrophy, and concha bullosa), as well as the severity of pathological findings, were noted.
The gathered data were subjected to Chi-square test analysis, and quantitative data were presented as mean ± standard deviation, utilizing SPSS 22 software for analysis. All procedures that involved human participants adhered to the ethical guidelines established by the institutional or national research committee (IR GUMS.REC.1394.350) of Guilan University of Medical Sciences, and were in compliance with the 1964 Helsinki declaration and its subsequent modifications, or ethical standards of comparable equivalence.
This research incorporated a total of 672 subjects, with females constituting 87.6% (579 patients) and males, 12.4% (83 patients). The sample population exhibited a mean age of 25.91 ± 6.45 years, with the age range spanning from 18 to 56 years. A considerable proportion of the participants were found to fall within the age range of 21 to 30 years. The findings further revealed that the majority of the participants had no pre-existing health conditions, while a minuscule 0.6% reported associated illnesses. Approximately 71% of the patients exhibited issues in both the septum and the lateral nasal wall (Figure 1).
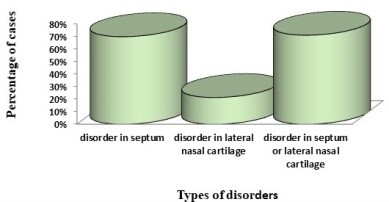
Figure 1. Prevalence of disorder in nasal septum and lateral nasal wall in candidates of septorhinoplasty
There was an absence of detectable septum or lateral nasal wall disorders in 29% (195) of the subjects. Out of the 672 participants slated for septorhinoplasty, 469 presented with a disorder of the nasal septum. A total of 1388 disorder instances were identified amongst these 469 patients. The most prevalent septum irregularity was a deviation in the maxillary crest (28.5%), followed by a spurred vomer, found in 24.6%. Only 143 patients reported a disorder in the lateral nasal wall, with 230 instances of lateral nasal cartilage disorders detected. Lower turbinate hypertrophy had the highest prevalence amongst lateral nasal wall disorders at 46.9%, with concha bullosa coming in second at 39.2%. Concomitant septoplasty was performed on 60% of the rhinoplasty candidates (Table 1).
Table 1. Distribution of disorders in nasal septum and lateral nasal wall in candidates of septorhinoplasty
| Disorder | N(%) | |
| Disorder in the septum | septal perforation | 6 (0.4) |
| Deviation of caudal septum | 211 (15.2) | |
| Maxillary crest deviation | 394 (28.5) | |
| Severe deviation of septum (need to be reconstructed with graft) | 203 (14.6) | |
| Dislocation of columella | 147 (10.6) | |
| Fracture in the cartilaginous septum | 85 (6.1) | |
| spurred vomer | 342 (24.6) | |
| Total | 1388 (100) | |
| Disorder in the lateral nasal wall | Lower turbinate hypertrophy | 108 (46.9) |
| Middle turbinate hypertrophy | 32 (13.9) | |
| concha bullosa | 90 (39.2) | |
| Total | 230 (100) | |
The employment of the Chi-square test was instrumental in ascertaining the correlation between the age groups of the subjects and the incidence of severe septum deviation, fracture in the cartilage septum, and lower turbinate hypertrophy. Notably, significant associations were detected in relation to each of these variables, as indicated by the respective values of P=0.004, P=0.033 and P=0.014. (Table 2).
Table 2. Frequency of disorders in nasal septum and lateral nasal wall in septorhinoplasty candidates in different age groups
| Disorder | Younger than 20 | 21-30 | 31-40 | Older than 40 | Total | p-value |
| Septal perforation [n (%)] | 0 (0) | 4 (1) | 1 (0.8) | 1 (5) | 6 (0.9) | 0.15 |
| Deviation of caudal septum [n (%)] | 32 (22.4) | 125 (32.8) | 46 (35.9) | 8 (40) | 211 (31.4) | 0.053 |
| Maxillary crest deviation [n (%)] | 73 (51) | 233 (61.2) | 75 (58.6) | 13 (65) | 394 (58.6) | 0.193 |
| Severe septum deviation [n (%)] | 27 (18.9) | 134 (35.2) | 37 (28.9) | 5 (25) | 203 (30.2) | 0.004 |
| Columellar dislocation [n (%)] | 30 (21) | 78 (20.5) | 33 (25.8) | 6 (30) | 147 (21.9) | 0.49 |
| Fracture in cartilage septum [n (%)] | 9 (6.3) | 53 (13.9) | 18(14.1) | 5 (25) | 85 (12.6) | 0.033 |
| Thoracic vomer [n (%)] | 67 (46.9) | 193 (50.7) | 72 (56.2) | 10 (50) | 342 (50.9) | 0.49 |
| Lower turbinate hypertrophy [n (%)] | 13 (9.1) | 76 (19.9) | 16 (12.5) | 3 (15) | 108 (16.1) | 0.014 |
| Middle turbinate hypertrophy [n (%)] | 5 (3.5) | 19 (5) | 6 (4.7) | 2 (10) | 32 (4.8) | 0.62 |
| Concha bullosa [n (%)] | 15 (10.5) | 59 (15.5) | 15 (11.7) | 1 (5) | 90 (13.4) | 0.26 |
Discussion
Investigation of nasal anatomy in preparation for surgical procedures is a common theme in rhinoplasty research. There have been numerous studies centering on the embryology and evolution of the nasal septum. However, a comprehensive exploration and depiction of nasal septum anatomy are rarely found, possibly due to the consistent clinical success of septoplasty and the assumption that the anatomy in question is broadly understood. The most extensive body of work in this field has been contributed by Rio Takahashi, with primary emphasis on growth, function, and causation of septal irregularities (18).
The nasal septum is pivotal in the development of the nasal and paranasal regions. It acts as an epiphyseal platform that originates from the facial skeleton. The potential for increased septal misalignment, alteration of the chondrovomer joint shape, or the occurrence of a septal perforation may arise due to the disconnection that exists between the three constituents of the adult nasal septum, namely the septum cartilage, the perpendicular plate of the ethmoid, and the vomer (19). Septoplasty is a crucial element of septorhinoplasty, the objective of which is to reconstruct the nose both for aesthetic and functional purposes (20).
As per Blaugrund's 1989 research, it was found that 20% of the population exhibited non-traumatic septum deviation (21). This percentage rose to 44% as evidenced by Earwalker's study conducted in 1993 (22). Our current investigation, based on a sample of 672 septorhinoplasty candidates, identified nasal septum disorders. Out of 469 patients, a total of 1388 issues were discovered. The most common nasal septum irregularity was maxillary crest deviation (58.6%), followed by spurred vomer (50.8%), and deviation of the caudal septum (31.3%). In contrast, only 143 patients presented with lateral nasal wall disorders, with the majority of these linked to lower turbinate hypertrophy (16.07%). This study established a significant correlation between the age groups of the candidates and the occurrence of septum and lateral nasal wall disorders.
Liu and team documented that the mucosal enlargement of the inferior turbinate on one side, coupled with the concurrent decrease of the bony portion of the turbinate on the opposite side, leads to imbalances in the positioning of the inferior turbinate. This, in turn, influences distinct ventilation patterns. They firmly urged avoiding interference with the atrophied side while addressing the enlarged turbinate through lateralization or mucosal diminution techniques (23).
Rehman and co-authors identified a growth in the occurrence of nasal septum deviations and posterior anomalies with age. Notwithstanding, the proportion of septal abnormalities fluctuates with age. The likelihood of septal irregularities escalates post nasal injury, and surgical intervention may be warranted to alleviate these circumstances (24).
Kayalioglu and his group found paradoxical curved middle concha in 12.22% (11 cases), concha bullosa in 28.88% (26 cases), nasal septum deviation in 22.22% (20 cases), and Haller cells in 5.55% (5 cases) of patients diagnosed with sinus pathology. In contrast, among patients devoid of sinus disease, 7.31% (6 cases) exhibited paradoxical curved middle concha, 26.83% (22 cases) concha bullosa, 12% (10 cases) nasal septum deviation, and 3.65% (3 cases) Haller cells (25).
In a separate investigation in Zagreb, abnormality prevalence stood at 28.8% across children and adults (26). Another comparable study by Adeel and his team, where the average age of the patients was 31 ± 13.15, showed one malformation observed exclusively in 16 patients (20.7%). Two disorders were detected in 18 patients (23.3%), and over three instances of irregularities and malformations were seen in 6 patients (7.7%) (27).
Yousem and colleagues undertook a study examining 100 CT scans, discovering that patients showing a high degree of sinus opacity tended to have a more severely deviated nasal septum (DNS) and unicate process (28). In a study of 202 patients who had undergone functional endoscopic sinus surgery (FESS), Bolger identified anatomical changes in 14.9% of the cases (29). An investigation by Deron, Clemant, and Derde into the impact of septal deviations and septal surgery on tubal function indicated that tubal function is improved through surgical correction of the septum (30).
Miandia and team proposed a seven-type classification for deviated nasal septum (DNS) in 1995, exploring the link between rhinosinusitis and septal anomalies. They suggested that this DNS classification sheds light on the connection between rhinosinusitis and the significance of septal disorders in causing rhinosinusitis (31). In an analysis of 22 scans, El. Shazly et al. identified associated irregularities in 49.7% of the instances. These comprised of 5 bilateral (22.7%) and 1 unilateral (4.5%) sinus ethmomaxilary, concha bullosa (13.6%) (1 unilateral and 2 bilateral), and two cases of bilateral bulla ethmoidalis (9%). (32).
A study by Roozbehani and others involved examining 65 patients with symptoms of sinusitis. They found that septal deviation was the cause of mucosal contact in 12 patients (18.5%). Septum perforations were found in seven patients (12.1%) and septum bullosa in two patients (3.1%). Paradoxical curved middle turbinate was discovered in three patients (4.6%). The most frequent anomaly found was middle turbinate concha bullosa, occurring in 19 patients (29.3%) (33).
In another study, Zinreich and team found unilateral concha bullosa in 34 patients (45%) and bilateral concha bullosa in 44 patients (55%) (34). Meanwhile, Zielnik-Jurkiewicz and colleagues conducted a study focusing on nasal disorders in children and adolescents. They diagnosed nasal septum deviation in 34% of the patients, with septal deformities occurring in 29% of girls and 37% of boys. There was a notable correlation between the patients' age and the type of nasal septum anomalies. In children who had experienced nasal injury, a deformed nasal septum was present in 66.66% of the cases (35).
Conclusion
In summarizing, the findings of our study align with the preponderance of previous investigations, noting septum deviation as the most prevalent condition. Given that every variation bears significance to the surgical process, it is essential that each case be independently examined prior to surgery to effectively address respective pathologies.
Acknowledgements
The financial support for this research was generously provided by the Guilan University of Medical Sciences, under the aegis of the Deputy of Research and Technology.
Funding
The financial support for this research was generously provided by the Guilan University of Medical Sciences, under the aegis of the Deputy of Research and Technology.
Conflicts of Interest
The authors assert without reservation that there exists no conflict of interest in connection to this investigation.
Received: 2022/09/1 | Accepted: 2023/01/28 | Published: 2023/06/26
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |